Simplify Management of Senior Living Operations
Proactively manage communities with analytics, insights, and connected software.
By centralizing all your work and using powerful reporting capabilities, you’ll quickly see what’s working and what isn’t so you can finally get ahead of issues before they become huge problems. Plus, you’ll give your team actionable insights into how to most effectively manage your business so there’s more time to focus on residents and your bottom line.
Our mobile-friendly solutions are built with your staff’s responsibilities in mind. Reports, dashboards, notifications and more will keep your team on top of every day-to-day task from large to small. Whether it’s back office operations, medication administration, or planning your meals and programming, these responsibilities can pile up or get overlooked without the right tools in place.
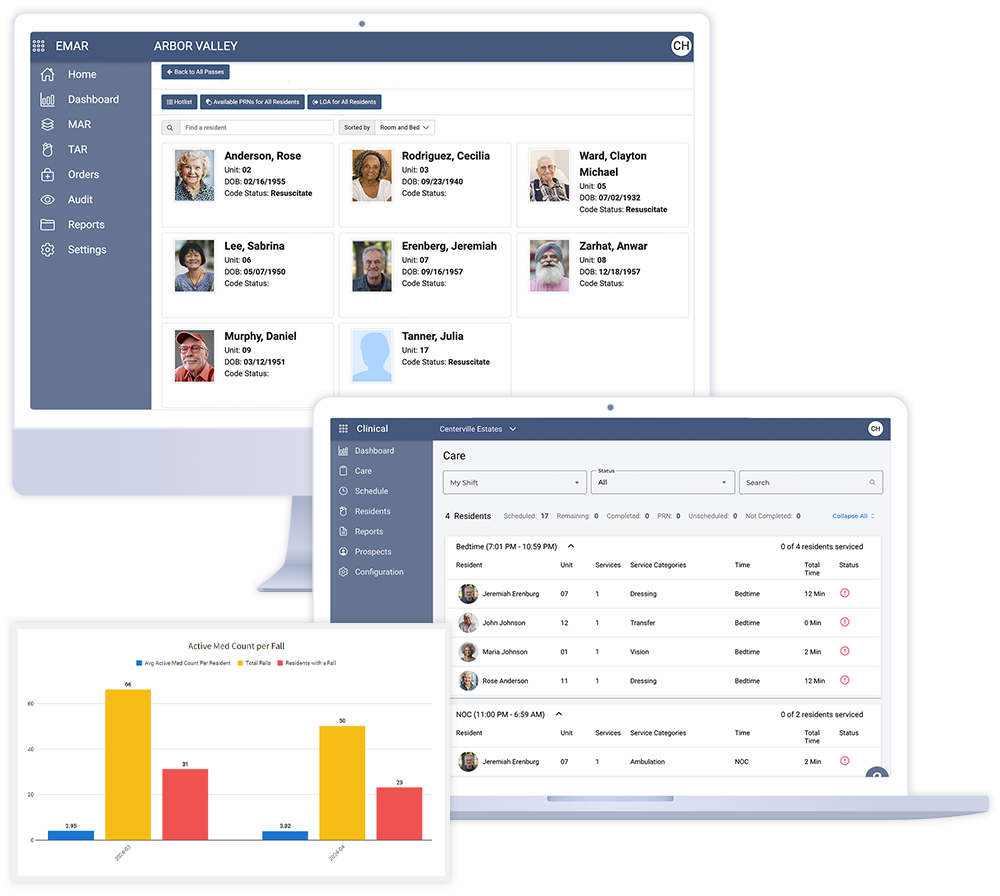
Eldermark's centralized platform streamlines operations, boosts revenue and care, simplifies tasks, and enhances resident outcomes
Hours back each month for Nurses
Hours back each month for staff while providing better coverage and care
Hours back each month for C-Suite
Data Management
Efficiently manage your data and gain insightful analytics so nothing goes unnoticed.
Organization-level view of the business, incorporating data from all platforms to identify performance gaps and opportunities, then prescribe actions
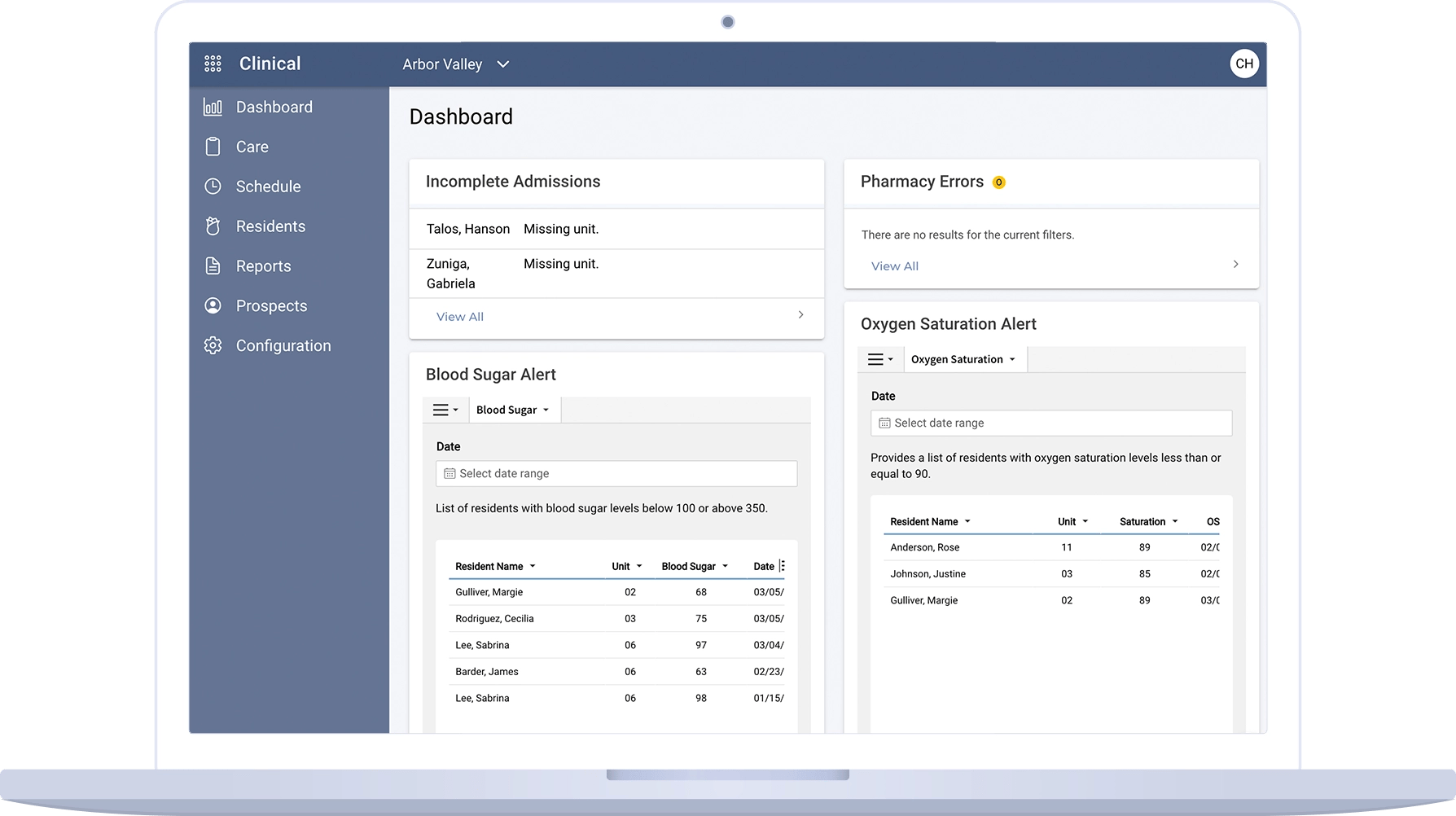
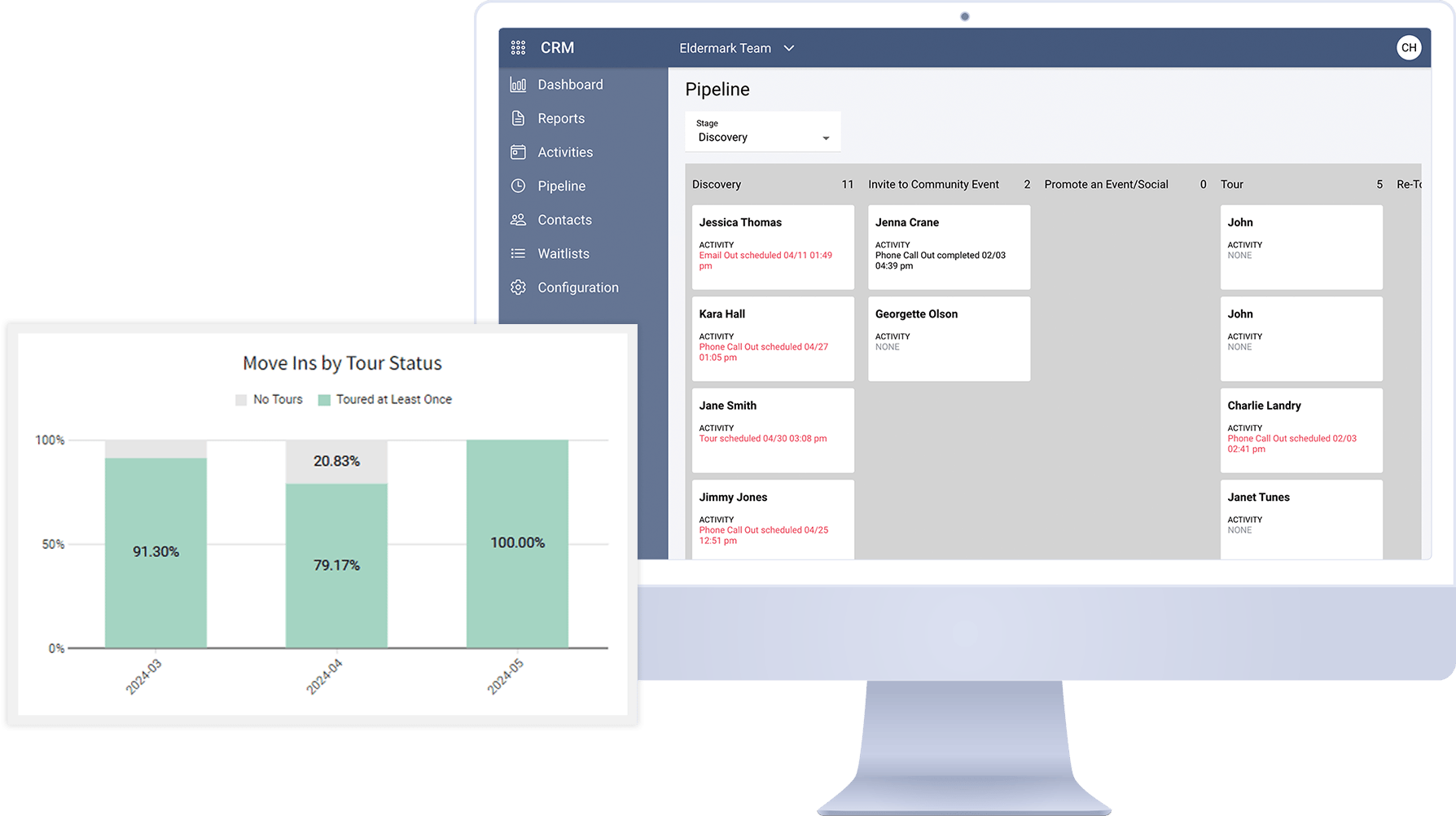
Operational Standardization & Efficiency
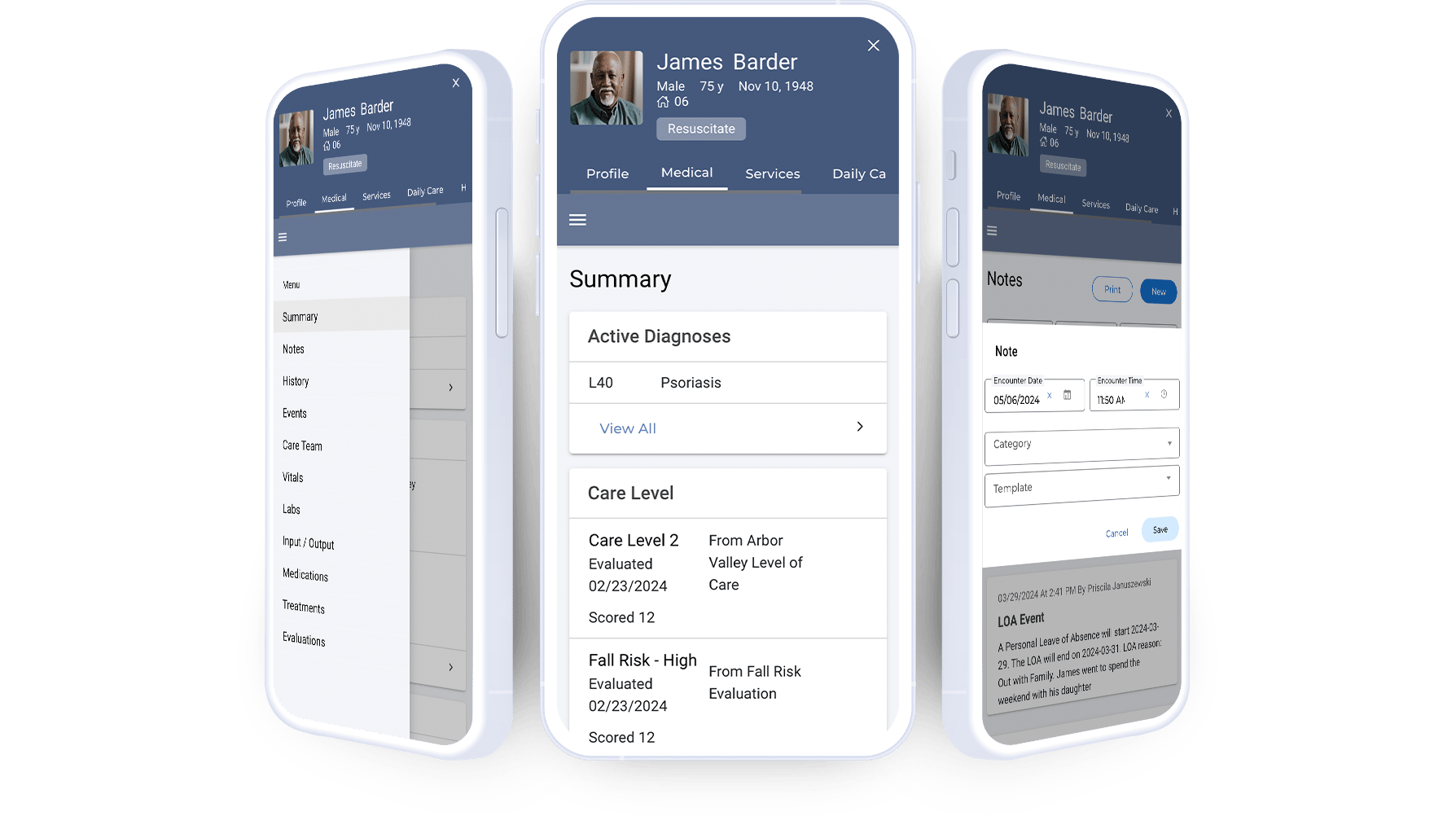
Take back time in your day to put towards more important matters. No more hard copy admin work – Eldermark can automate your paperwork and help you electronically manage health records, medication administration, medical charts, employee shifts, and more.
Improve the safety, health, and satisfaction of residents and employees, and get the complete picture of your residents' well-being
Increase efficiency and accuracy for caregivers with one-touch medical charting
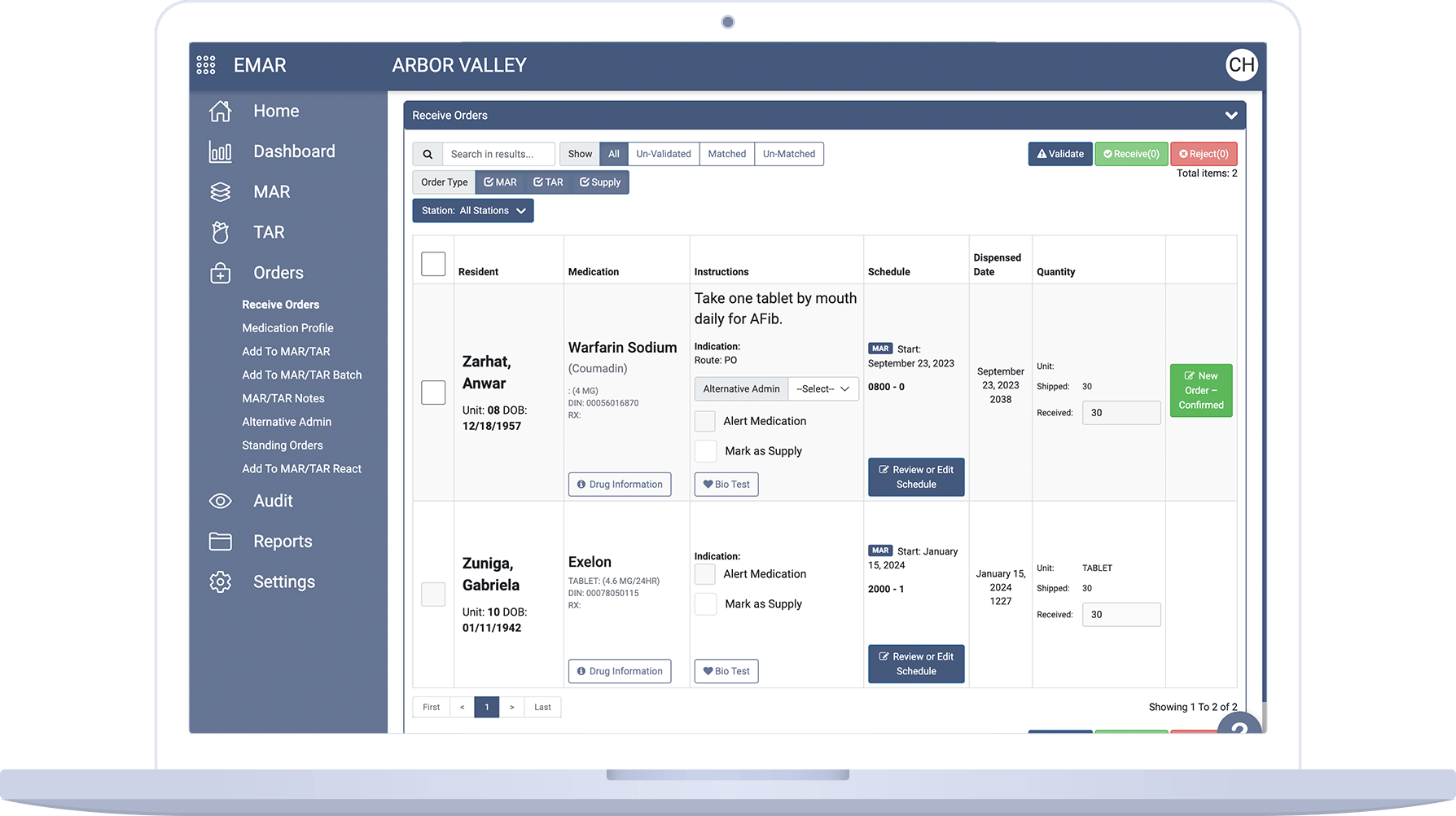
Regulatory Compliance Support
Eldermark is committed to meeting regulatory requirements and enhancing clinical interoperability. As a HIPAA-compliant software, Eldermark ensures security and confidentiality of resident data.
Eldermark's integration with Surescripts provides senior living communities with essential support for regulatory compliance regarding residents' protected health information (PHI). By ensuring compliance with state laws and offering secure access to a health information exchange Eldermark empowers providers to uphold privacy standards and access up-to-date health information efficiently.

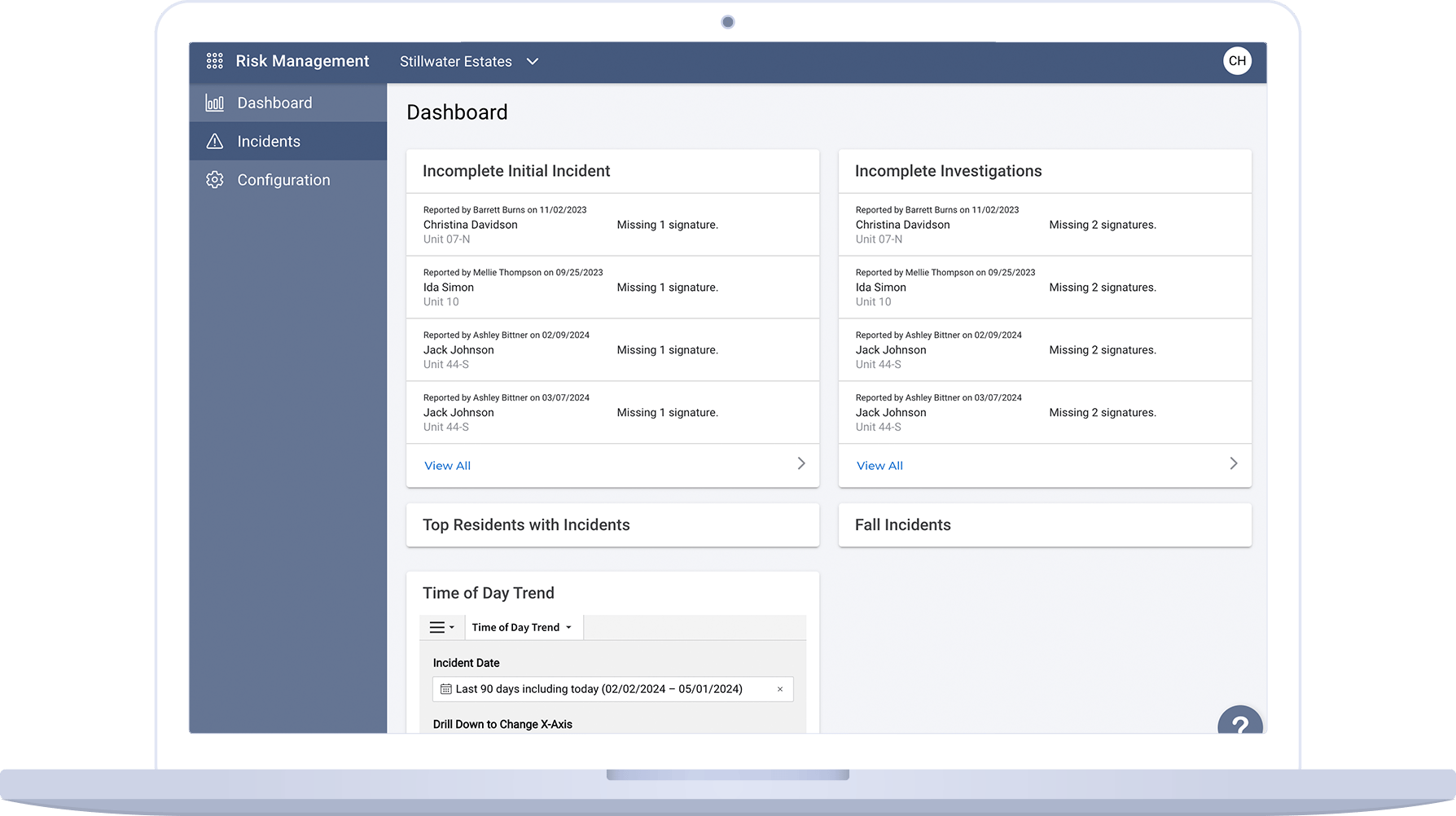
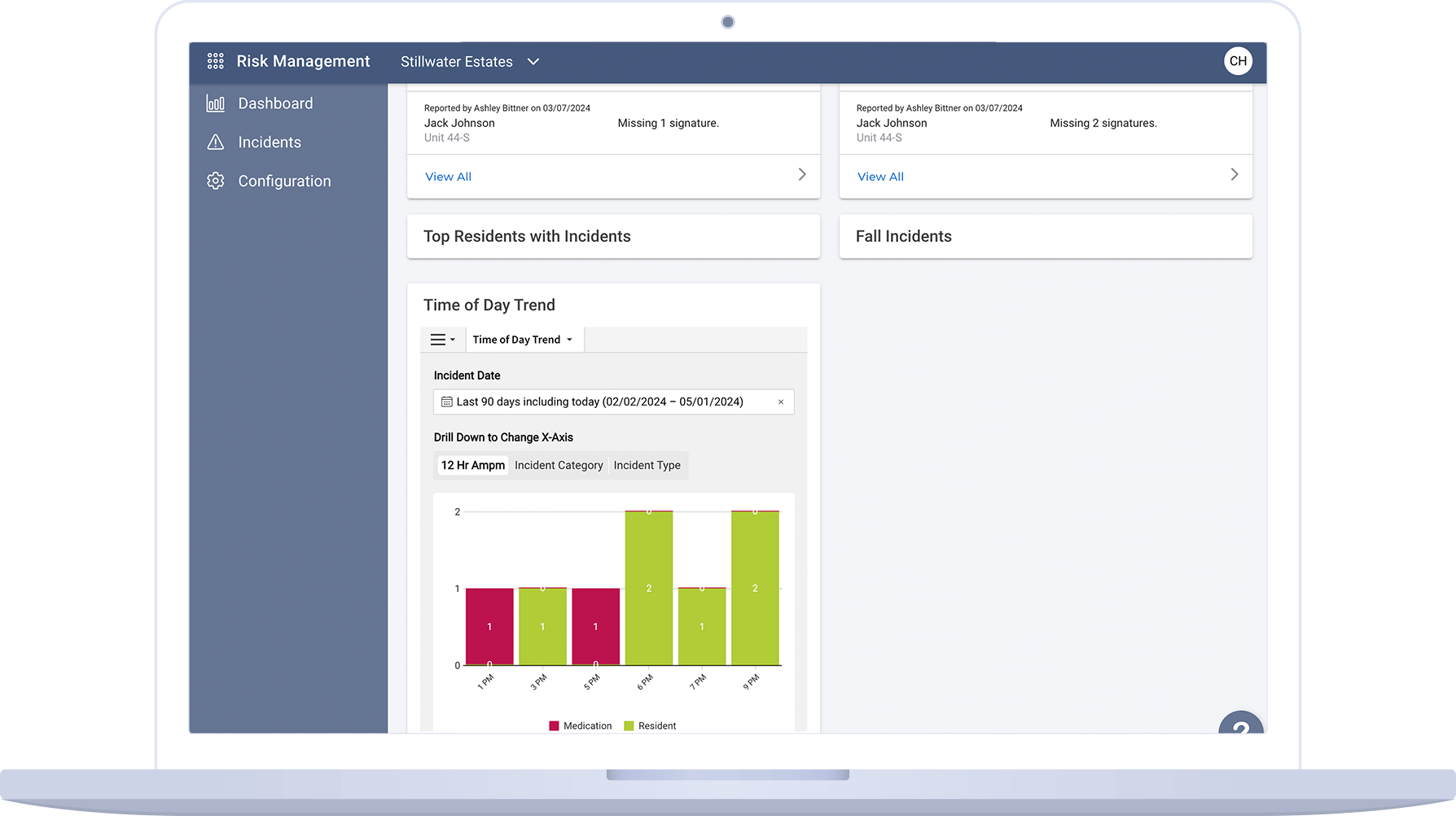
Clinical Risk Management
Enhance resident safety and operational efficiency by leveraging the Risk Management app. Our integrated risk management program provides actionable insights, streamlined incident documentation, and detailed analytics to optimize operations, reduce costs, and ultimately improve resident well-being.
Identify risk analysis opportunities and respond to resident condition changes in real-time
Track and respond to resident condition changes as they come up
“Eldermark has been a huge time saver for our company. It has so many awesome functions. Pretty much if you can think it, Eldermark has a way to make it happen and they are always improving on the user experience.”

Quality Auditor
Medium provider of assisted living services
Want to standardize operations and improve efficiencies?
Take a look at these resources and insights from Eldermark.

How Eldermark’s Business Model Design Helped Faribault Senior Living Grow
By right-sizing care plans and implementation of ElderSmarts Analytics and software, Eldermark helped Faribault Senior Living address their top operational challenges and set them up to reach their financial and business goals!

Eldermark Partners with Peerlytics for Infection Control Management in Senior Living Communities
Eldermark, an acclaimed healthcare technology provider for the senior care industry, today announced a new partnership with Peerlytics designed to help senior living communities better manage infection control and antibiotic stewardship for their residents.

