What Is an eMAR? — A Complete Guide for Assisted Living Operators
Medication management in assisted living is harder than it looks on paper.
"I can't be on the floor 24/7. I need to know when a med pass is late without physically walking the building."
Every clinical leader reading this has heard some version of that sentence. In assisted living, medication management is a visibility problem, a workflow problem, and a compliance problem. The right eMAR solves all three.

What is an eMAR?
An eMAR, or electronic medication administration record, is the digital system used to schedule, document, and track medication administration. It gives your team a live, consistent record of what medications are due, when they are due, and what happened during the med pass.
In assisted living, the right eMAR does more than replace paper. It helps staff manage med pass more consistently, creates a clearer record of what happened, and gives clinical leadership better visibility into medication activity across the building.
The real question is not just what an eMAR is — it is what happens in your building without one. In assisted living, medication management is not just a documentation problem. It is a visibility problem, a workflow problem, a compliance problem, and often a communication problem between care staff, pharmacy, and clinical leadership.


Why eMAR matters in assisted living
Medication management in assisted living is harder than generic healthcare content usually makes it sound. Residents are moving in later. Acuity is rising. Medication lists are longer. Orders are more complex.
A single med pass may involve routine medications, PRNs, vitals-based parameters, time-sensitive administration windows, refill coordination, and psychotropic documentation expectations. On top of that, many communities rely on med techs to carry out medication workflows that still require consistency, accuracy, and accountability. That is a difficult system to run well on paper.
The best assisted living eMAR systems help staff follow the right process in the moment, help clinical leaders see what is happening without walking the building, and help communities stay audit-ready without digging through stacks of paper after the fact.
For assisted living communities, eMAR is not just a technology upgrade. It is an operating system for one of the most risk-sensitive parts of the building.
How does an eMAR work?
A caregiver logs in and sees what medications are due for each resident — schedule, administration details, and any related instructions. As the med pass happens, the caregiver documents in real time, along with any refusal, delay, omission, or required follow-up. That creates a live, time-stamped record tied to the person who completed the task.
Workflow that guides care in the moment
A paper MAR can show a medication was due. It cannot guide the staff member through the process consistently, provide surface-level visibility across shifts, or help a clinical leader see what is happening community-wide without manually reviewing charts.
Documentation that clarifies the next step
When documentation is clean, time-stamped, and centralized, staff can see what was completed, what still needs attention, and what changed since the previous shift. That reduces the friction that builds when handwritten notes and disconnected systems carry too much of the workload.
Medication education standards →Visibility without walking the floor
An eMAR helps clinical leadership answer questions faster: Was the medication administered? Was it late? Was it refused? Is a refill needed? Is this an isolated issue or a broader pattern? That visibility changes how quickly a team can respond and how confidently a clinical leader can stand behind the documentation.
What is medication reconciliation →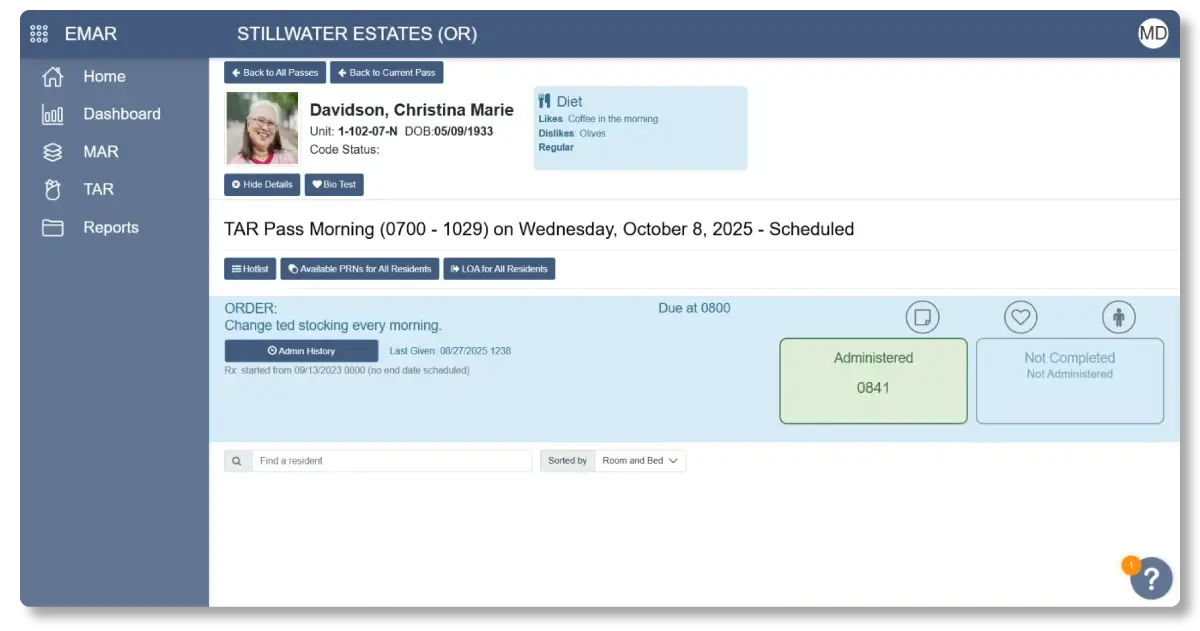
Why paper MAR breaks down in assisted living
Paper MAR rarely fails all at once. It fails in pieces.
A handwritten update is missed. A pharmacy change is not carried forward correctly. A refill issue sits too long. A signature makes the process look complete even when the medication was not available. A month-end reconciliation takes hours and still leaves uncertainty about what actually happened.
That is why paper remains such a fragile system in assisted living. Residents often manage multiple chronic conditions, long medication lists, and more medically complex regimens than communities were navigating several years ago. The gap between clinical complexity and who is actually administering medications is part of the challenge. That is exactly the kind of gap paper does not help close.
When those gaps go unnoticed, the result is often an adverse drug event — a preventable harm that paper-based workflows are poorly equipped to catch.
Paper doesn't alert or surface patterns quickly.
A clinical leader cannot see what is happening during the med pass without physically reviewing charts. There is no mechanism to flag late medications, surface emerging issues, or escalate concerns in real time.
Paper can't support clinical oversight in real time.
When the medication pass is happening, there is no live view of what was administered, what was missed, or what needs follow-up. Leadership remains reactive — only able to respond after the fact.
Paper creates the appearance of accountability.
The record can appear complete even when the underlying workflow was not. A signature does not mean the medication was available. That gap between documentation and reality is where compliance risk lives.
Benefits of eMAR for assisted living communities
A strong eMAR changes more than one task. It improves the reliability of the whole medication workflow.
Better medication accuracy
When staff can see what is due, document in real time, and follow a structured workflow, the chances of missed steps, overlooked follow-ups, and documentation confusion go down. Barcode medication administration adds another verification layer at the point of care.
Clearer staff workflows
A paper process asks people to remember too much. An eMAR reduces that burden. Instead of relying on handwritten notes, verbal updates, and later reconciliation, staff work from a live record that is easier to follow and easier to update.
Faster documentation
Documentation always has to happen. The question is how painful it is. When the record is digital, centralized, and easier to update, staff spend less time chasing paper and more time on resident care.
Stronger compliance readiness
Medication documentation is where communities have to prove what happened, when, and who completed it. An eMAR makes that trail easier to retrieve, easier to interpret, and easier to trust when a surveyor is in the building.
Better communication with pharmacy
When orders change, medications run low, or refills are needed, staff should not depend on workarounds. A connected eMAR reduces handoff gaps, keeps medication storage and order tracking in sync, and gives staff a clearer path to action.
Better line of sight for clinical leaders
Clinical leaders do not need another pile of records to review after the fact. They need to know what is happening while there is still time to act. Visibility across residents, shifts, and buildings — without walking the floor — is what a well-implemented eMAR delivers.
See how Eldermark eMAR works in an assisted living building.
eMAR and compliance: why survey readiness matters
"It collects data and allows us to easily see trends and capture areas we can focus on quality improvement."
Kayla G.
That is not just a convenience issue. It is a compliance issue.
Assisted living is state-regulated, and medication administration documentation remains one of the clearest places where communities have to demonstrate consistency and control. The medication safety officer role is central to that process, and eMAR is one of the primary tools that role depends on. When the documentation trail is messy, incomplete, or difficult to retrieve, the risk is not just operational — it becomes regulatory.
Paper MAR slows retrieval. It introduces interpretation problems. It leaves too much room for the record to appear finished when the workflow behind it was not.

Survey-ready documentation should be:
That is what an eMAR supports. That is what paper cannot consistently deliver at the level of complexity assisted living communities are now carrying.
What to look for in an eMAR system
Not every eMAR solves the same problem. Some systems digitize the record but leave the workflow fragmented. Some look fine in a demo but create new burden once the community is live. Here is what matters most when you are evaluating options.
Ease of use for med techs and nurses
If the frontline team does not trust the system, they will work around it. The workflow has to be intuitive for the people actually administering medications — not just usable in a demo.
Real-time visibility for clinical leaders
You should be able to see what happened today — not just after someone runs a report. That visibility matters for late meds, missed tasks, resident-specific issues, and broader process breakdowns.
Clean documentation trail
Time-stamped entries, clear user attribution, and a structure that supports audit readiness without heavy manual interpretation. The record should be easy to trust the first time a surveyor looks at it.
Pharmacy integration
If pharmacy communication still depends on separate manual updates, the risk does not disappear when you go digital. A connected workflow is one of the most common failure points in disconnected systems.
What is e-prescribing →EHR connectivity
Medication administration does not live on an island. If the eMAR does not connect cleanly with the broader resident record, your clinical team still ends up stitching the story together across systems.
Reporting and oversight tools
Clinical leaders should not have to dig for basic answers. A good eMAR supports fast review, cleaner oversight, and a clearer picture of what is happening across residents, shifts, and buildings.
For a breakdown of the different architectures on the market, see The Five Types of eMAR Systems for Senior Living →
Why integration matters more than features
A lot of buyers get pulled into feature comparisons too early. But in assisted living, the larger issue is often architecture.
A standalone eMAR may remove paper, but it can still leave your team doing the integration work manually. Medications in one place, care plans in another, pharmacy communication somewhere else. The building still operates through handoffs — it just does so digitally. That is not the same thing as a connected workflow.
An integrated eMAR changes what your clinical team can actually see and do:
That is the difference between a system that documents med pass and a system that helps the building run better.

What implementation should look like
Communities hesitate not because they think paper is better, but because they have been burned before. They worry the transition will be chaotic, staff will resist it, and the building will carry the implementation burden without enough support. That concern is legitimate.
A good eMAR implementation should feel structured, role-specific, and operationally grounded — not like the community is being asked to become its own software onboarding team.
1. Moving from paper MAR
2. Training by role
3. Go-live support
4. Adoption in the first 30 days
The case for eMAR: what clinical leaders need to know
The clinical leader who needs to make the case for eMAR usually has a stronger argument than they think. This is not a quality-of-life purchase for the care team in isolation. It is a building-level clinical decision with direct implications for risk, compliance, and the capacity of your team to do their jobs well.
The four dimensions below are where the argument is clearest — and where the cost of staying on paper is most visible.

Medication workflows carry too much consequence for a fragile system
A community without real-time visibility, a strong documentation trail, and cleaner staff guidance is carrying more clinical risk than it needs to. When something goes wrong, the documentation is the first thing a surveyor asks for.
What is a drug utilization review →Survey readiness becomes fragile when documentation is hard to trust
When documentation is hard to retrieve, hard to trust, or hard to interpret, survey readiness becomes much more fragile. eMAR strengthens the trail when the building needs to demonstrate what happened, when it happened, and who was responsible.
Time on paper is time taken away from residents
Time spent on paper reconciliation, duplicate documentation, and manual follow-up is time taken away from resident care. The more efficient the medication workflow becomes, the more clinical capacity your team gets back every day.
Disconnected workflows create preventable problems at every handoff
A disconnected medication workflow creates preventable problems between care staff, pharmacy, and clinical leadership. A shared, accurate record reduces that friction at every handoff point.
Read the case study →Frequently asked questions about eMAR
eMAR stands for electronic medication administration record.
A MAR is the medication administration record — the document used to track what medications a resident receives. An eMAR is the digital version of that record, with the added ability to alert staff, surface patterns, and support real-time oversight. See Medication Administration Records for a full breakdown of the paper-based record and where it typically falls short.
An EHR, or electronic health record, is the broader clinical record for a resident that includes assessments, care plans, notes, and more. An eMAR is typically one component within or connected to an EHR, focused specifically on medication administration. In some platforms they are integrated. In others they operate separately and require manual reconciliation. See EHR vs. EMR vs. eMAR: The Key Differences to Know for a full breakdown.
It can be. In many senior living environments, eMAR works alongside or inside the broader EHR workflow so medication administration is connected to the rest of the resident record.
They use eMAR to improve medication workflow consistency, strengthen documentation, reduce paper burden, support compliance, and give clinical leadership better visibility into med pass activity across the building.
Yes. A strong eMAR supports clearer, time-stamped documentation that is easier to retrieve and review during incidents, audits, and surveys. State requirements vary by care setting — consult your state's assisted living regulations for specifics on documentation standards.
The eMAR Glossary covers key terms in depth. For role-specific clinical context, see resources on medication administration records, medication reconciliation, and medication education standards in senior living.
Go deeper on medication management in assisted living
This page is the hub for the Eldermark eMAR content cluster. The pages below cover the topics introduced here in greater depth.
eMAR Glossary
Key terms for medication administration, electronic health records, and assisted living clinical workflows — defined for operators and clinical leaders.
Read more → Reference GuideMedication Administration Records
What the paper-based MAR actually involves, how it is used in assisted living communities, and where the gaps typically appear.
Read more → BlogEHR vs. EMR vs. eMAR: The Key Differences to Know
A breakdown of how these three terms relate and why the distinction matters for clinical teams evaluating technology in senior living.
Read more → BlogThe Five Types of eMAR Systems for Senior Living
A breakdown of the different eMAR architectures on the market — what each one does, and what it does not solve.
Read more → BlogeMAR Integrations: The Benefits of Creating One Centralized System
How centralizing eMAR with related systems reduces tech overload, improves workflows, and connects medication administration to broader resident care data.
Read more → Case StudyWhy eMAR? A Case Study
A real example of what a connected eMAR workflow looks like in an assisted living community — before, during, and after implementation.
Read more →Built for assisted living communities that need more than a digital replacement for paper.
Eldermark's eMAR is designed to help communities simplify medication administration, strengthen clinical documentation, and give clinical leadership the visibility they need to stay ahead of problems — not just respond to them.
Because medication administration in assisted living does not operate in isolation, Eldermark's eMAR connects to the broader resident record, giving clinical teams a more complete and accurate picture of care across the building.
For clinical leaders, that means a system that helps guide the work at the point of care, reduces the documentation burden on frontline staff, and creates a documentation trail that holds up when it needs to.
Schedule a Demo
See Eldermark eMAR in action.
Connect with our senior living team. We will walk through the medication workflow, show you how clinical oversight works in real time, and answer your questions about implementation.